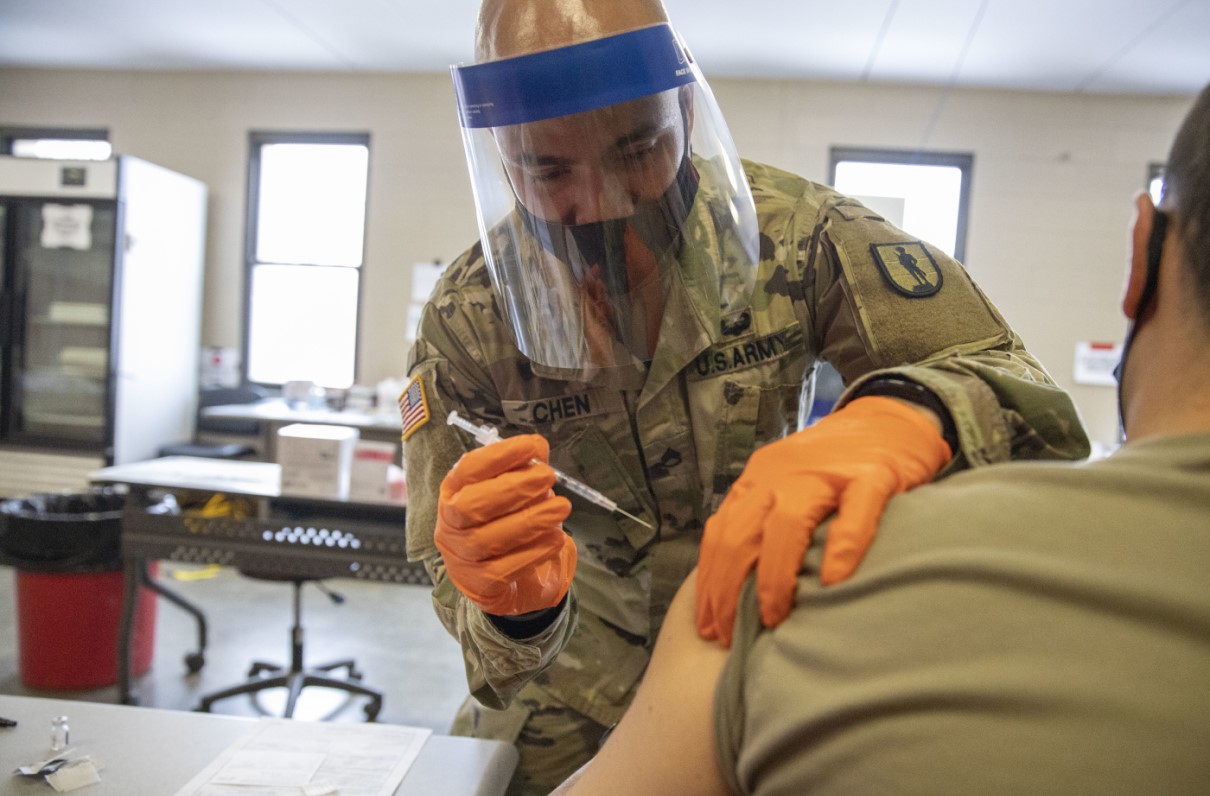
Some coverage changes and rule exceptions designed to make securing care easier during the COVID-19 pandemic expired May 11 along with the end of the federally declared public health emergency. And while many of the changes have to do with COVID diagnosis and treatment, others will affect a wider swath of individuals who receive care from various health agencies.
Here’s a quick look at some updated coverage guidance, plus links to find out more specific information related to your unique health concerns.
TRICARE
- COVID-19 Testing: Beneficiaries may have a cost share for testing. TRICARE will continue coverage of medically necessary tests ordered by authorized providers; TRICARE For Life users can learn about more testing changes to their Medicare coverage below.
- Clinical Trials: TRICARE overage of COVID-19 clinical trials sponsored by the National Institute of Allergy and Infectious Diseases ended April 10, but those already enrolled in trials as of that date will remain covered.
- Skilled Nursing Facility (SNF) Coverage: TRICARE requires a three-day hospital stay before a beneficiary can be admitted to a skilled nursing facility. That requirement had been lifted during the COVID-19 emergency, but was back in place as of April 10.
Medicare
- Over-the-Counter (OTC) COVID-19 Tests: These tests are no longer free to Medicare Part B beneficiaries. Lab tests ordered by an authorized provider remain free, and some Medicare Advantage plans may continue to cover the OTC tests. Check with your plan for details.
- COVID-19 Treatments/Vaccines: Antivirals such as Paxlovid and Lagevrio will remain free, as will COVID vaccines. However, this policy may change when the government stops “purchasing or distributing” these materials, according to the Department of Health and Human Services (HHS). Changes on this front could come “in the coming months.”
- Skilled Nursing Facility Coverage: Similar to TRICARE (above), Medicare stopped requiring a three-day qualifying hospital stay before covering a beneficiary’s time in a skilled nursing facility under Part A. That requirement is back in place as of May 11, though stays which began prior to May 11 will remain covered. Again, Medicare Advantage coverage of this situation varies; check with your plan for details.
- Telehealth: Most Medicare expansions of telehealth care undertaken during the pandemic will remain in place through 2024, thanks in part to legislation extending these changes. One notable exception: Regular, routine telehealth home care is no longer covered under Medicare’s hospice benefit. TRICARE For Life (TFL) beneficiaries who use telehealth should monitor for potential changes to Medicare coverage policy in 2025 and beyond; TRICARE has made some telehealth coverage expansions permanent and these apply to TFL beneficiaries but, for services not covered by Medicare, TRICARE becomes first payer and the TRICARE deductible and cost shares apply.
- More Information: Download a PDF from the Centers for Medicare and Medicaid Services; visit the HHS website; learn more about COVID-19 coverage at Medicare.gov.
VA Care
- COVID-19 Vaccines: The shots remain free for veterans eligible to receive VA health care, but the end of the health emergency removes VA’s authority to vaccinate caregivers, spouses, or veterans not eligible for VA care.
- Caregiver Visits: In-person visits as part of VA caregiver assistance programs – home-care assessments, for instance – already have resumed in most cases. The end of the pandemic emergency marks a return to in-person visits across the board; participants in the Program of Comprehensive Assistance for Family Caregivers (PCAFC) should be contacted by the VA regarding this changeover.
- Telehealth: VA Video Connect remains the official platform for VA telehealth visits, with Webex also authorized in limited cases. The VA will limit the use of other platforms as of May 11. A recent extension of a pandemic prescription rule will allow many VA beneficiaries to continue receive drugs prescribed by out-of-state telehealth providers. Read more here.
- More Information: Read a full breakdown of VA benefits affected by the Public Health Emergency, including travel reimbursement guidance and assistance for homeless veterans.
Stay Up to Date With MOAA
Keep up with the latest news on your medical care at MOAA.org/news, and visit MOAA’s TRICARE Guide and TRICARE Toolkit for answers to frequently asked questions about retiree health benefits.
MEDIPLUS® TRICARE Supplement
Works hand-in-hand with your Select or Prime Plan. Count on valuable protection.